Wolverton Station’s Emma Jackson with Karryn Dolan and husband Peter in Cairns Hospital after Karryn’s recovery from a massive heart attack.
Karryn Dolan should be dead. On a dark and rainy Cape York night, the 59-year-old suffered a massive heart attack on a remote cattle station. Doctors in Cairns certainly didn’t think she’d make it. They even told her family to prepare to say goodbye. But two weeks later, Karryn is now walking, talking and even smiling. Cape York Weekly editor Matt Nichollswrites how the stars aligned for Karryn that night …
SIX hours. That’s how long it took for Karryn Dolan to reach a hospital after going into cardiac arrest on the night of December 30, 2021.
Every doctor you speak to will say that it’s a miracle she’s still alive.
They might be right. But there were a number of people who played a key role in her survival that deserve the credit.
They are Karryn’s angels.
* * * * *
IT was a balmy Cape York night and there had been some rain around as a tropical low came across the Peninsula. It’s typical weather for that time of year.
Peter and Karryn Dolan have been coming to Cape York for years. The Cairns couple love camping, fishing and pig hunting.
Peter’s second cousin is Neville Jackson from Wolverton Station, so they often bring their small off-road caravan and make base at the cattle property, located about two hours south of Weipa.
Thursday, December 30 was a fairly typical day for them.
“We’d been out hunting for pigs and were on our way back in when we saw a pig near the dam about 500 metres from the house,” Peter said.
“It was dark at this point, probably around 8 o’clock.
“The dogs chased after the pig and luckily they got it fairly quickly. They baled it up in no time.
“But it threw one of the dogs off and unbeknownst to me, the dog raced off to Karryn who was with the quad bike.
“I yelled out: ‘where’s Whiskey’ and heard Karryn say: ‘Whiskey’s with me’.

It’s a bit different in the day time but this is where Karryn collapsed on Wolverton Station.
“So I started walking towards her and all of a sudden I saw her on the ground. It was probably just seconds after she collapsed.”
Peter said he didn’t know his wife had suffered a heart attack.
“I thought she had tripped over. There were some vines around,” he recalled.
“But then she wasn’t moving.”
He tried to call his son to alert Emma Jackson – Neville’s wife – but couldn’t get through.
There is no phone reception on Wolverton unless you are close enough to be connected to the homestead’s satellite internet.
“I had started CPR but then I had a decision to make. No one knew we were out there so I put Karryn on the back of the quad and raced to the house,” Peter said.

The gunyah at Wolverton Station.
Emma knew something was wrong immediately.
She could hear the quad bike approaching and Peter was shouting and honking the horn.
“I thought it might have been one of the dogs – that a pig had injured one of them,” she said.
It was soon clear to Emma and her family that it was Karryn who needed attention.
This is where the stars begin to align for her.
* * * * *
TWO years earlier, the Royal Flying Doctor Service had donated a defibrillator to Wolverton Station and trained Emma how to use it.
In a previous life, Emma had studied psychology in the UK and ended up staying in Australia after falling in love with Neville – she nursed him back to health after he suffered horrific burns in a bush fire almost two decades ago.

Bull catcher, snake wrangler, station boss, ambulance driver – there isn’t much that Neville Jackson can’t do.
But that’s another story.
The fact is Karryn had a station manager with advanced first aid training, as well as a defibrillator on hand.
“I remember Emma telling me a year earlier that they had a full RFDS kit and a defib,” Peter said.
“The only thing I could do was to get her to Emma as quickly as possible.”
* * * * *
WHEN Karryn was brought to the back of the Wolverton homestead – more of a gunyah, really – she was not breathing and didn’t have a pulse.
“She was lying on the back of the quad and her eyes were open, but she looked gone,” Emma said.
“It took three shocks with the defib and intermittent CPR to get a pulse back.
“She was still on the back of the quad bike and then we eventually moved her to a towel on the floor.
“No one thought about whether she was going to make it or not. We had to do everything we could until the ambulance arrived. We were determined not to lose her.”
Once they had a pulse, Emma and Peter continued to provide CPR to Karryn, hoping that she would fight to survive.
Paramedic Paul Spinks says he got the call for help at 8.17pm.
Knowing the complexities of the case, he went looking for help.
“In a remote town, you would normally get the police. I tried to get them but they were on another job,” he said.
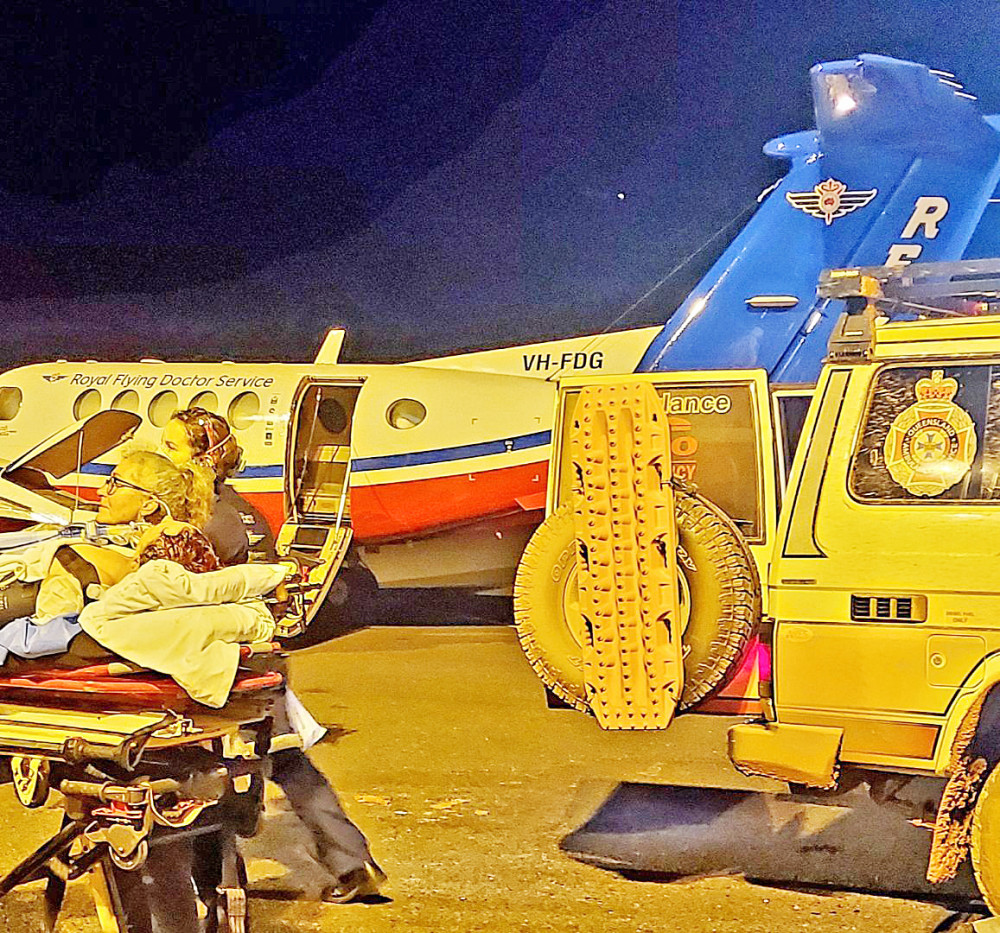
Dr Rebecca Brady and flight nurse Michelle Ball attend to Karryn Dolan on the tarmac at Coen Airport.
“Coen is a single officer paramedic station so on the bigger jobs we scramble around for support.
“There was a single nurse on call at the clinic. I got hold of her and told her I needed help.
“There was one other nurse in town so he got called and came in to cover the town while I took Sandy out to Wolverton.”
Paul admitted that he was driving to Wolverton thinking the worst possible outcome.
“When you’re in Brisbane or on the Gold Coast you like to get to those jobs within 10 minutes.
“Down there, you’d have eight ambulances following each other and a police presence, too.
“When I got the call I’m told that CPR is in progress and I’m thinking that I’m an hour and 15 minutes away – there’s no way the patient will be alive when we get there.”
On a largely unsealed road from Coen to Wolverton, the trip is about 85km.
Add pouring rain and it’s not a simple drive, even with a purpose-built four-wheel-drive ambulance.
“Because of the torrential rain. and the road conditions, we had to slow down to 40km/h at one point,” Paul recalled.
“You couldn’t see. At one stage we had to pull over and clean the headlights with our face masks to give us better visibility.”

Paramedic Paul Spinks played a critical role in Karryn’s survival.
Paul and Sandy arrived at the house at 9.31pm.
Somehow, the CPR had started to work and Karryn was breathing again, although she was not in a good way.
“It was initially quite exciting for us because it gave us hope,” Emma said.
“But she was quite ill and was vomiting and groaning.
“She went into this reflexive mode with her arms flailing about and we couldn’t settle her. It was quite traumatic.”
Karryn’s condition required Paul and Sandy to stay in the back of the ambulance to keep her stabilised for the trip to Coen Airport, where they were to meet an RFDS plane.
“When you’re remote you need to find the most responsible person so I said to Neville and Peter ‘one of you needs to drive the ambulance’,” Paul said.
Peter said it was never going to be him.
“I would have driven too fast. Plus, Neville knows the road better than anyone,” he said.
So it was Neville who took the wheel – barefoot, of course – while Emma and Peter followed in a car.
* * * * *
GETTING air support was not a simple task.
Wolverton has an airstrip but no lighting, ruling out a night landing, while there were no available planes or helicopters at the time.
RFDS doctor Rebecca Brady was in Bamaga when she got the desperate call.
“There was a patient in Bamaga who had been waiting for a retrieval to Cairns and we finally got a window in the weather when we could make it up there,” she said.

A four-wheel-drive ambulance from Coen and an RFDS plane were critical in saving Karryn Dolan’s life.
“But as we were at the Bamaga Hospital I got a call from Retrieval Services Queensland, which is the overarching retrieval hub for the state – they coordinate the ambulance, helicopters and RFDS.
“They said there was a really sick patient in the Archer River area and we were the only asset in the area.
“They said ‘are you able to go there or do we need to task a jet from Brisbane?’, so it was only us who could go.”
They had to break the news to the Bamaga patient that she would not be going to Cairns and quickly raced back to the airport to fly to Coen to meet the ambulance.
“It was all systems go as Karryn needed us ASAP,” she said.
“I spoke to Paul and before we took off – she was critically unwell in the back of the ambulance.”
Dr Brady said she was lucky to be flying with experienced flight nurse Michelle Ball, who helped prepare the plane for Karryn’s treatment.
They landed in Coen at 11.41pm and were taxiing towards the small terminal when the ambulance arrived.

Dr Rebecca Brady spends a week each month working for the RFDS in Cape York due to her love of the Far North.
Within minutes they had set up a tarp and an impromptu medical centre to treat Karryn.
“We assessed her and immediately realised that despite the best efforts of Emma, Peter and Paul, she was still in a really critical condition,” Dr Brady said.
“She wasn’t fully conscious and was agitated. She had been low on oxygen for a long period and her heart wasn’t working properly.”
In the flight retrieval business, there are quick decisions to be made.
“We had to toss-up between ‘stay and play or scoop and go’,” Dr Brady said.
“That’s the reality of the situation and, in this case, we had to get her as stable as possible before we put her on the plane.”
Under the floodlight, flying ants made treatment even more difficult, but the RFDS team managed to put Karryn into an induced coma.
“It wasn’t raining but it was very muggy and we were wearing full PPE so it wasn’t ideal working conditions,” she said.
“When we got her into the plane and were in transit we were able to perform some blood tests and get her prepared for the team at Cairns Base Hospital.
“Thankfully she didn’t arrest again or we would have lost her, for sure.”
The plane left Coen at 1.21am and arrived at Cairns Airport just over an hour later.
“We got Karryn onto a stretcher and we all travelled in the back of the ambulance to the hospital,” Dr Brady said.
“The emergency department had been informed of the case a couple of hours earlier so they were well prepared.”
Peter says it was all a blur for him, with memories of the night still emerging as he speaks more about the event.

Peter and Karryn Dolan last year.
He was lucky to be able to jump in the plane with Karryn – the RFDS can’t always accommodate family members due to weight loads and the amount of care required in the aircraft.
It would have been an eight-hour drive in the middle of the night to get to Cairns Hospital.
“I’m so grateful I could be there,” he said.
“When she went into the ED I had to sit outside and wait, but once she was put into ICU (intensive care unit) they were quick to get me to her.”
* * * * *
DESPITE all the effort that had gone into keeping Karryn alive and getting her to hospital, Peter said he still wasn’t optimistic in the early hours of that Friday morning.
“I thought there might be a problem because of the timeline and how long she went without breathing,” he said.
Those fears were confirmed later that morning when doctors from the ICU told Peter to start preparing for the worst-case scenario.
“The next morning they basically told us to prepare for the end of life,” he said.
“It was sort of expected but it still hit really hard.”
Peter and Karryn’s five children all live in the Far North and scrambled to be by her bedside.
“Everyone did their best to be there and we had the kids, the in-laws and the grandchildren in the family room at the hospital,” he said.
“Because of COVID, we could only have two people in the room at any one time so they were taking it in turns.”
He admitted that family members were saying goodbye.
* * * * *
THAT afternoon, however, there was a change in Karryn’s condition.
“I wasn’t in the room but (daughter) Sarah was playing her some music – Luke Combs is her favourite artist – and I think the nurse said something about her breathing changed,” Peter said.

Country singer Luke Combs is Karryn’s favourite artist.
“She was taking breaths of her own and you could see her nose flare as she started to breathe.
“Then she squeezed Sarah’s hand. The nurse asked if she could hear anything and she opened her eyes.
“We knew then she was a chance to pull through.”
From that moment, Karryn has been improving each day.
“We did three laps of the ward today,” Peter said.
“There is still some short-term memory loss which we hope will get better, but she has been making big improvements.
“The people in ICU are still saying that it’s a miracle.”
* * * * *
A LOT of factors worked in Karryn’s favour that night.
Everyone involved said the defibrillator was the most important piece of the puzzle.
“If we didn’t have the defib we know she would be dead,” said Emma, who added, “if anything, I’m glad it happened on Wolverton because we had the equipment and the training. Not every cattle station has a defib.”
Strong first aid training and instincts also paid off.
Emma and Peter didn’t give up on Karryn and kept administering CPR, which bought her time for the ambulance to arrive.
The fact an ambulance was in Coen was another game-changer.

Having a defibrillator on Wolverton Station saved Karryn’s life.
Five years ago, there was no Queensland Ambulance Service in Coen, just a clinic with nurses.
When the state government finally built a station in the community, the service was initially for the dry season only, when the population peaks in the region due to the number of tourists.
But funding was later guaranteed to make Coen a year-round operation, which definitely worked in Karryn’s favour.
Then there’s the Archer River.
At the time of writing, the Archer River is flowing above the causeway, meaning road access to Coen is blocked.
Two weeks ago, however, the road was clear, albeit wet and muddy. It would have taken more than two hours for the ambulance to arrive at Wolverton if they had to send one from Weipa.
The next factor that worked in Karryn’s favour was the ability for the RFDS to redirect services from Bamaga.
With no other aerial capability in the Far North, if Dr Brady had been unreachable, the outcome would have surely been different.
Then there is the treatment by both paramedic Paul and the RFDS team which stabilised Karryn enough to get her to Cairns.
A well-prepared emergency unit at Cairns Base Hospital did its bit, as did the ICU crew.
The final piece was the love of Karryn’s family.
Told to say goodbye, the warmth of her children and grandchildren was the final ingredient.
Who knows what would have happened if Luke Combs’ music wasn’t played?
“This really is a feel-good story and one that needs to be told to highlight the importance of having the right first aid equipment,” said Emma.
“We need to use this as a lesson so that people invest in defibrillators and other life-saving equipment.”

A happy ending – Emma Jackson with Karryn Dolan.
Peter said the RFDS had ultimately saved his wife’s life.
“We got very lucky. Everything just sort of fell into place,” he said.
“If you think about it; if it happened at home in Cairns it might have been a different outcome because it might have taken an ambulance 10 minutes to arrive with a defib.
“At Wolverton, we had the defib on her within a few minutes.”
Dr Brady said she was thrilled to be a part of such a feel-good story.
“There were so many cogs in the machine that night that worked in Karryn’s favour,” she said.
“Having the AED (automated external defibrillator) there, having good CPR – all of it ultimately saved her life,” she said.
“We teach the chain of survival and for non-medical people to kick into action like that was amazing.”
Dr Brady is based in Brisbane but has a close connection to the Far North, having been born in Cairns and raised in the region.
She spends one week each month in Cape York, working with the RFDS to treat patients.
“In remote Australia we work in such resource-poor environments and still get the job done,” she said.
“This is a great example of how people should be trained in CPR and first aid.
“Karryn has survived an event that would have a survival rate of 10 per cent in the best of conditions.”
Paul has been working for 16 years as a paramedic but has only just started working remotely.

Karryn is now recovering in Cairns Base Hospital and doctors hope she will be back home soon.
He works on a week-on, week-off roster out of Coen and says that Karryn’s story will go down as the best of his career.
“You’ve got to pull out every card in the book to manage scenes like this,” he said.
“Up here you’re all alone.”
Remote work has some benefits not found in bigger cities.
“It’s extremely rewarding,” Paul said.
“You don’t often hear of the outcome. It’s so personal.
“I have been in touch with Emma, been in touch with Peter and have been getting sent photos and updates.
“I feel like Karryn is my aunty.”
Emma said she hoped this would inspire Cape York residents to take the time to learn first aid training and attend the RFDS field days.
“Judith from the RFDS is a real champion out here and organises field days that focus on different first aid each time,” she said.
“That training will end up saving a life.”
She also paid tribute to James, the Triple Zero operator who was with her and the family on the phone while Karryn was getting CPR on the floor at Wolverton.
“He was so calm and clear in his instructions,” she said.
“I was told that when the call came in his manager was called in and there was a team supporting James on the phone.
“I got in touch with Josh Milne from QFES in Cairns and passed on a thank you note to be given to James.
“It was a real team effort.”